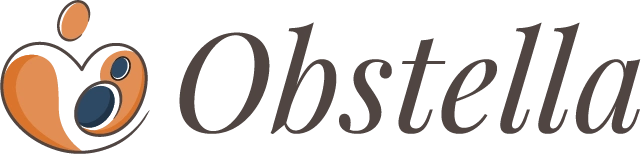Waiting for mammogram results can be a nerve-wracking experience, filled with anxiety and a whirlwind of “what-ifs.” The language used in these reports often feels like a foreign dialect, peppered with medical jargon that can be more confusing than clarifying. Terms like “BI-RADS,” “calcifications,” and “asymmetries” can leave you feeling overwhelmed and uncertain about your health.
This comprehensive guide aims to demystify the process, translating complex medical terminology into plain English. We’ll walk you through the timeline for receiving results, break down the key components of your report, explain the critical BI-RADS scoring system, and outline the potential next steps. Our goal is to empower you with the knowledge to understand your mammogram results, reduce your anxiety, and facilitate more productive conversations with your healthcare provider. Understanding mammograms is an essential part of breast health and cancer prevention.
The Timeline and Transparency: What to Expect When Waiting for Mammogram Results
How long does it take to get my mammogram results?
The waiting period for mammogram results can vary significantly depending on the facility, the type of mammogram (screening vs. diagnostic), and legal requirements. In the United States, the Mammography Quality Standards Act (MQSA) requires facilities to send patients their results in writing within 30 days. However, most facilities provide results much sooner, often within a few days to two weeks. If you haven’t heard back within two weeks, it’s reasonable for a patient to follow up with the imaging center or your doctor’s office.
For a screening mammogram, a radiologist reads the images at a later time. If the results are normal and no signs of cancer were found, you’ll typically receive a letter in the mail. If there’s a potential area of concern, you’ll receive a phone call to schedule a follow-up appointment for a diagnostic mammogram. In the case of a diagnostic mammogram, the radiologist often reviews the images in real-time and may discuss the preliminary findings with you on the same day.
Deconstructing Your Breast Imaging Report: A Jargon Decoder
Understanding Breast Density: Categories A through D
One of the first things mentioned in a mammogram report is breast density. Dense breast tissue (composed of more fibrous and glandular tissue than fat) appears white on mammograms, as do tumors. This can make it harder to detect cancer. It’s also important to note that some benign (not cancer) breast conditions are denser than fat and appear white on imaging. Breast density is categorized as follows:
- Category A: Almost entirely fatty. Breasts are composed almost entirely of fat. Cancer detection is easiest in this group.
- Category B: Scattered areas of fibroglandular density. There are scattered areas of density, but the majority of the breast is fatty.
- Category C: Heterogeneously dense. More than half the breast is composed of dense tissue, which could obscure small masses.
- Category D: Extremely dense. The vast majority of the breast is dense tissue, making it difficult to see through and increasing the risk of missing a cancer.
Many states now have laws requiring facilities to notify patients if they have dense breasts, as they may benefit from supplemental screening, such as a breast ultrasound or MRI for comprehensive breast health monitoring.
The Big Three Confusers for Dense Breasts: Masses, Calcifications, and Asymmetries
These are the three most common findings that require further investigation:
- Masses: A mass is a space-occupying lesion seen in two different projections. The report will describe its shape (e.g., oval, round, irregular), margin (e.g., circumscribed, spiculated), and density. Irregular shapes and spiculated (spiky) margins are more concerning.
- Calcifications: These are tiny deposits of calcium in the breast tissue. They are very common and usually benign (non-cancerous). Macrocalcifications are larger, coarse deposits often due to aging or old injuries. Microcalcifications are smaller and can sometimes be a sign of early cancer. Their morphology and distribution (e.g., clustered, linear) are key indicators for the radiologist.
- Asymmetry: This is when an area in one breast looks different from the same area in the other breast. If it’s new or has changed since a previous mammogram (a “developing asymmetry”), it will require a workup.
BI-RADS Category Designation Explained: Your Score, Risk Assessment, and Management Protocol
The Breast Imaging Reporting and Data System (BI-RADS) is a standard scoring system radiologists use to communicate mammogram results. Your mammogram results are scored from 0 to 6, providing a clear framework for understanding your breast health status.
BI-RADS 1 and 2: Negative and Benign Findings (Routine Screening)
- BI-RADS 1: Negative. There is nothing to comment on. Your breast tissue appears normal and the findings are negative. Your mammogram is normal with no signs of cancer, masses, or other abnormalities. Recommended follow-up is routine screening.
- BI-RADS 2: Benign Finding. There is a definite benign finding (like a benign calcification or cyst), but it is not cancerous. These findings are harmless and do not increase your cancer risk. Recommended follow-up is also routine screening.
BI-RADS 0 and 3: The Anxiety Zone (Incomplete and Probably Benign)
- BI-RADS 0: Incomplete. The radiologist needs more information. This is common after a first-time screening mammogram or if prior images are not available for comparison. It requires additional imaging, such as a diagnostic mammogram or ultrasound. This does not mean cancer, only that more views are needed.
- BI-RADS 3: Probably Benign. The finding has a very high probability (>98%) of being benign. A short-interval follow-up is recommended, typically a repeat mammogram in 6 months to ensure the area is stable.
BI-RADS 4 and 5: Suspicious and Highly Suggestive of Malignancy
- BI-RADS 4: Suspicious Abnormality. Findings are suspicious enough to warrant a biopsy. This category may be subdivided: 4A (low suspicion), 4B (moderate suspicion), and 4C (high suspicion).
- BI-RADS 5: Highly Suggestive of Malignancy. Findings have a classic appearance of cancer (>95% probability). A biopsy is strongly recommended to confirm the diagnosis.
Note: BI-RADS 6 is reserved for cases where a biopsy has already confirmed cancer, and imaging is being done for treatment planning.

Actionable Next Steps: A Comparative Guide to Diagnostic Follow-Up Tests
If your report comes back with a BI-RADS score of 0, 3, 4, or 5, you will need some form of follow-up. Here are the most common procedures used in breast health evaluation and cancer prevention:
Diagnostic Mammogram and Breast Ultrasound
- Diagnostic Mammogram: More detailed than a screening mammogram. The technician takes additional views, including magnification views for calcifications or spot compression views to better define a mass.
- Breast Ultrasound: Uses sound waves to create images. Helpful for determining if a mass is solid or a fluid-filled cyst. It can also be used as supplemental screening for dense breasts.
When is a Breast MRI Necessary?
A Breast MRI uses magnets and radio waves to create detailed images. It is typically used for:
- High-risk screening (strong family history or genetic mutation like BRCA)
- Evaluating extent of disease after a cancer diagnosis
- Further assessment when an abnormality is not well visualized on mammogram or ultrasound
Understanding Biopsies: Core Needle vs. Fine-Needle Aspiration
If imaging tests cannot rule out cancer, a biopsy is performed to extract a tissue sample for analysis. This is the only way to definitively diagnose breast cancer.
- Fine-Needle Aspiration (FNA): Uses a very thin needle to withdraw fluid or cells. Often used to confirm a simple cyst.
- Core Needle Biopsy: Uses a larger needle to remove small tissue samples. This is the most common biopsy type and is often done with ultrasound, stereotactic mammography, or MRI guidance.
Managing Scanxiety: Your Emotional Roadmap for Waiting and Follow-Up of an Abnormal Mammogram
“Scanxiety,” or the anxiety associated with medical scans and waiting for results, is a real and valid emotional response. It’s important to have tools to manage stress during the waiting period.
Coping Strategies: Mindfulness and Controlled Worry
- Acknowledge your feelings: It is okay to feel scared or anxious.
- Practice mindfulness: Deep breathing, meditation, or gentle yoga can help reduce spiraling worries.
- Set aside “worry time”: Allow a short, specific daily window to focus on fears, then shift attention elsewhere.
- Stay informed, but avoid “Dr. Google”: Use reputable sources to avoid misinformation and increased anxiety.
Mammogram results explained: Decode BI-RADS scores, understand breast density, and learn what your findings mean. Get the clarity you need for informed decisions.
The “3 Questions to Ask Your Doctor” Checklist
When you discuss your results, being prepared can help you feel more in control. Write down your questions beforehand. Consider these three essential questions:
- Can you explain my BI-RADS score and what it means for my specific situation?
- What are the recommended next steps, and what are the risks and benefits of each?
- When can I expect the results of any follow-up tests, and how will I be notified?
Summary of Key BI-RADS Categories and Next Steps
Have questions about your reproductive health? Our providers at CWC Alabama are here to help you understand your options and feel confident in your care.
References
- American College of Radiology. (n.d.). ACR BI-RADS® Atlas. Retrieved from https://www.acr.org/Clinical-Resources/Reporting-and-Data-Systems/Bi-Rads
- American Cancer Society. (2023). Understanding Your Mammogram Report. Retrieved from https://www.cancer.org/cancer/breast-cancer/screening-tests-and-early-detection/mammograms/understanding-your-mammogram-report.html
- Komen, S. G. (2023). Breast Density. Retrieved from https://www.komen.org/breast-cancer/risk-factor/breast-density/